How Medical Coding Automation Is Transforming Clinical and Billing Workflows
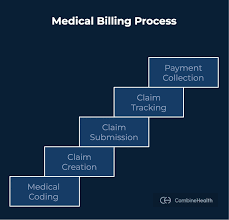
Medical coding links patient care directly to provider revenue. AI-driven coding automation reduced claim rejections by up to 40% in early adopter health systems during 2024-2025. It turns complex clinical information into billable data.
Manual processes are slow and introduce human error. This creates bottlenecks in both clinical and financial operations.
Healthcare organizations must improve coding accuracy and speed. Staff shortages and higher patient volumes increase pressure. Coding errors cause claim denials and payment delays. This strains financial health and staff resources.
Implementing automated medical coding addresses these core challenges. Intelligent software reviews documentation to suggest accurate codes. This technology cuts manual work and reduces errors. It lets human coders concentrate on complex, high-value cases.
This blog examines how coding automation changes key workflows. We detail its impact on clinical documentation. We analyze gains in billing efficiency and revenue cycle speed. We also cover practical strategies for implementation.
Addressing the Core Challenges of Manual Medical Coding
Manual medical coding is a resource-intensive and error-prone process. It depends heavily on individual coder expertise and recall. Coders must navigate thousands of complex, frequently updated code sets. This includes ICD-10, CPT, and HCPCS Level II codes.
Key limitations of traditional manual coding include:
- Productivity Constraints: Manual coding limits the number of charts a coder can process daily. This creates backlogs as patient volume increases.
- Inconsistency and Human Error: Coding decisions can vary between individuals. Fatigue or oversight can lead to missed or incorrect codes.
- Difficulty Scaling Operations: Hiring and training new coders to meet demand is costly and time-consuming. It is difficult to scale manual teams quickly.
- Compliance Risks: Keeping pace with annual code updates and payer-specific rules manually increases audit risk. Missing a new guideline can cause widespread claim issues.
These challenges contribute directly to revenue cycle inefficiency. They slow down the entire claim submission and payment process. Organizations experience longer accounts receivable days as a result.
How Automation Integrates with Clinical Documentation
Medical coding automation begins at the point of clinical documentation. Modern platforms use natural language processing (NLP) to read physician notes. The AI extracts key clinical facts, diagnoses, and procedures from unstructured text.
This creates a direct link between documentation and coding:
- Real-Time Code Suggestions: As a clinician documents, the system can suggest relevant codes. This happens within the electronic health record (EHR) workflow.
- Clinical Documentation Improvement (CDI): Automation flags incomplete or nonspecific documentation proactively. It prompts clinicians for clarification before the visit ends.
- Reduced Retrospective Queries: The need for coders to query physicians days later decreases significantly. This accelerates the coding cycle.
This integration transforms coding from a separate, downstream task. It becomes a concurrent part of the clinical documentation process. Clinicians receive immediate feedback on documentation quality. This leads to more accurate and complete medical records from the start.
read more : https://techlokesh.info/
Transforming Billing Efficiency and Revenue Cycle Speed
Automation’s most significant impact is often seen in the billing office. It accelerates the entire revenue cycle from chart closure to claim submission. Cleaner claims move to payers faster and with greater accuracy.
Measurable improvements in billing efficiency include:
- Faster Chart Turnaround Time: AI can process over 1,000 charts per minute for initial review. This eliminates coding backlogs that delay billing.
- Higher First-Pass Clean Claim Rates: Automated systems apply payer rules in real-time. They achieve higher clean claim rates by preventing errors upfront.
- Reduced Denial Rates: Pre-submission scrubbing identifies potential denial reasons. This can lead to a greater reduction in claim denials.
- Accelerated Cash Flow: With faster, cleaner claims, payments arrive sooner. Organizations often reduce A/R days.
Billing staff spend less time on manual claim corrections and resubmissions. Their focus shifts to managing exceptions and following up on aged accounts. This represents a better use of skilled revenue cycle talent.
Key Features of Effective Medical Coding Automation
Not all automation platforms deliver the same results. Effective solutions share several critical capabilities. These features determine the technology’s real-world impact on workflows.
Healthcare leaders should look for these key features:
- High Accuracy Across Specialties: The AI should maintain accuracy rates of 96% or higher. It must cover a wide range of clinical specialties, ideally 36 or more.
- Seamless EHR Integration: The system must work within existing clinician and coder workflows. Deep EHR integration avoids disruptive application switching.
- Human-in-the-Loop Design: Automation should handle routine, high-volume cases autonomously. Complex charts should be flagged for expert coder review.
- Continuous Learning and Updates: The platform must update automatically with new coding guidelines. It should learn from auditor and coder feedback over time.
The best platforms function as collaborative intelligence tools. They augment the coding team rather than aiming to replace it entirely. This hybrid approach balances efficiency gains with necessary clinical oversight.
Implementing Automation: Strategy and Change Management
Successful implementation requires more than just installing new software. It involves careful planning around people, processes, and technology. A phased approach minimizes disruption and builds organizational buy-in.
A strategic implementation plan should include:
- Workflow Analysis and Integration: Map current coding and documentation workflows first. Design how the new technology will integrate without adding steps.
- Phased Rollout by Specialty: Start with one or two high-volume, lower-complexity service lines. Use this pilot to refine processes and train super-users.
- Targeted Training Programs: Train coders on how to work with AI suggestions and overrides. Train clinicians on how documentation impacts AI code suggestions.
- Performance Metric Establishment: Define clear KPIs for success before launching. Track metrics like coder productivity, accuracy, and claim turnaround time.
Change management is crucial for user adoption. Communicate the benefits clearly to both clinical and administrative staff. Position the technology as a tool to make their jobs easier, not as surveillance. Address concerns about job security openly and honestly.
Measuring the Impact on Clinical and Financial Outcomes
The value of medical coding automation should be measured in concrete outcomes. These span clinical, operational, and financial areas of the organization. Tracking the right metrics demonstrates return on investment.
Key performance indicators to monitor include:
- Coder Productivity: Measure charts coded per hour per FTE. Automation typically improves productivity.
- Coding Accuracy: Audit a sample of AI-coded charts against gold-standard manual reviews. Maintain accuracy at or above 96%.
- Claim Denial Rate: Track the percentage of claims denied for coding reasons. Expect reductions of 40% or greater.
- Average A/R Days: Monitor the time from service to payment receipt. Reductions of 30% or more are common.
- Clinical Query Reduction: Measure the decrease in retrospective queries to physicians. This improves clinician satisfaction.
Long-term benefits also include improved audit readiness and compliance. Automated systems create a clear audit trail for every code assigned. They apply rules consistently, reducing compliance risk across the organization.
Conclusion
Medical coding automation represents a fundamental shift in health information management. It moves coding from a manual, retrospective task to an integrated, intelligent process. This transformation delivers clear benefits across clinical and billing workflows.
Clinicians experience fewer interruptions from coding queries. They receive real-time feedback to improve documentation quality. Coding teams achieve dramatic productivity gains while maintaining high accuracy. The revenue cycle accelerates as clean claims move to payers faster.
The transition requires thoughtful strategy and change management. The focus must remain on augmenting human expertise, not replacing it. When implemented effectively, coding automation strengthens both financial performance and clinical documentation. It allows healthcare organizations to scale efficiently while reducing administrative burden.